What is the function of the prostate?
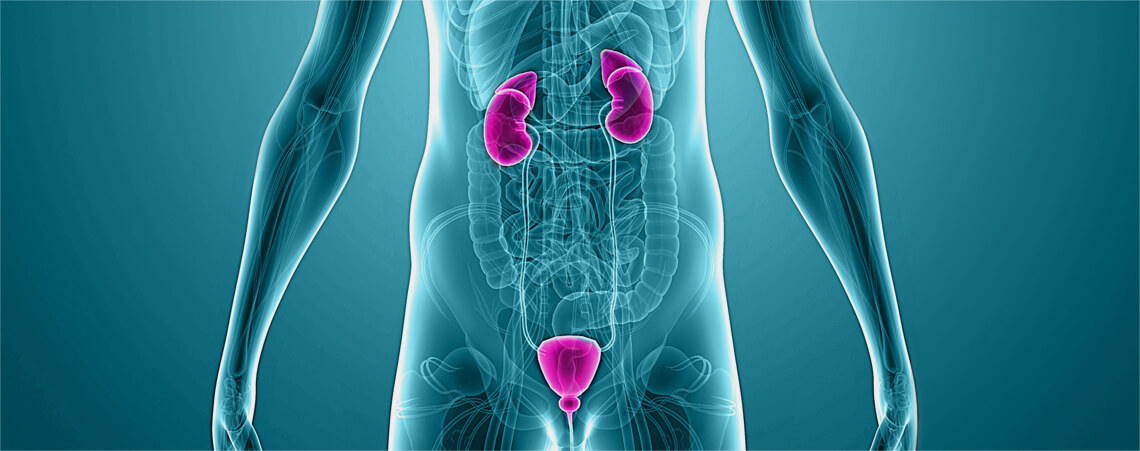
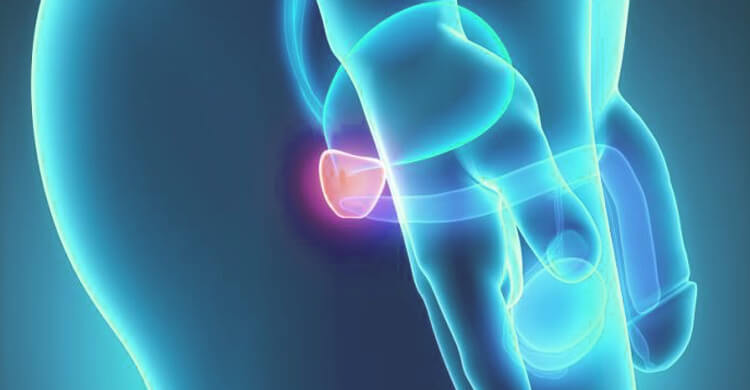
The prostate is a gland of between 15 and 20 grams (normal size) and is located immediately below the bladder and in front of the rectum. It produces and stores seminal fluid to protect and enrich sperm. The most common prostate diseases are benign (aging) hyperplasia of the prostate resulting in decreased urine flow, prostate infections, and prostate cancer, which is the number one cancer in men and the second largest cause of death from cancer for men from the USA.
Common symptoms of prostate diseases include:
- A need to urinate frequently, especially at night.
- Difficulty experienced while releasing urine or retaining urine.
- Weak or interrupted flow of urine. Painful or burning sensation during urination.
- Difficulty maintaining an erection.
- Painful ejaculation.
- Blood in urine or semen.
- Frequent pain or stiffness in the lower back, hips or upper thighs.
The prostate disorders we treat
Prostatitis
Prostatitis is an inflammation of the prostate gland, often resulting in swelling or pain, urination problems, sexual dysfunction, and general health problems, such as feeling tired and depressed. Prostatitis can be treated with dietary changes, antibiotics, and occasionally, surgery.
An enlarged prostate (better known as benign prostatic hyperplasia – BPH)
An enlarged prostate is common in aging men, with up to 90% of men over 80 presenting with this condition. BPH can be treated medicinally or through a common surgical procedure called a Transurethral Resection of the Prostate (TURP). During surgery a medical instrument called a resectoscope, which consists of a light, valves for irrigating fluid and an electrical loop is inserted through the tip of the penis into the urethra. The loop cuts tissue and seals the blood vessels. The removed tissue will be flushed into the bladder and out of the body through a catheter that is placed into the patient’s bladder through the penis.
Prostate cancer
Prostate cancer is the second most common cancer in men with 1 in 6 men likely to experience prostate cancer in their lifetimes. Small areas of cancer within the prostate are very common and may stay dormant (inactive) for many years making it very different from most other cancers.
Prostate cancer occurs when cells of the prostate begin to multiply out of control. Sometimes these cells may spread to other areas of the body, which in medical terms is known as metastasis. Prostate cancer is a slow growing cancer compared with other cancers and is usually diagnosed in the early stages before it starts to spread outside the prostate gland. However, it is possible that prostate cancer can be advanced when it is first diagnosed in men. This can also be the case for men who have previously been treated for early or locally advanced prostate cancer but whose cancer has recurred.